
200 Durand Street #208
St-Jérôme, Québec
J7Z 7E2 Canada

Wisdom teeth |
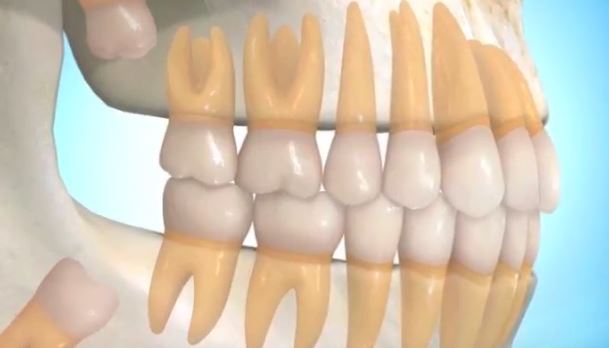
Why remove them?There are many reasons for extracting wisdom teeth.
It can be seen that there are many possible complications related to wisdom teeth. It should be known that the 3rd molars of the bottom cause more problems than those of the top. In addition, these problems increase in frequency after the age of 25 years. Even if you have no symptoms at the moment, it is best to extract the 3rd molars to prevent long term dental problems. Opinions may differ, however, with respect to preventive extraction. Some will prefer to monitor an asymptomatic tooth instead of extracting it, especially if the X-ray indicates a proximity between it and the lower alveolar nerve. Indeed, in the case where such proximity exists, caution is needed not to cause damage to the nerve. Finally, in some people, the available space and angulation of the tooth are optimal and allow a normal eruption. For these, it is of course useless to proceed with the extraction. |
How does the extraction of wisdom teeth take place?X-ray is very helpful to your surgeon for planning surgery. Depending on the inclination of the tooth, its degree of inclusion and its proximity to the inferior alveolar nerve, the procedure can be modified. The surgeon will opt for a simple extraction, if the tooth is present in the mouth, or a complex extraction if the tooth is included or semi-included. Complex extraction, also known as surgical extraction, involves the surgeon having to incise the gingiva, cut the jaw bone to release the tooth, and close the incision with stitches. Sometimes it may be necessary to cut the wisdom tooth into several pieces to remove it. In both cases, the patient can choose the option of anesthesia that suits him best. Some people prefer to sleep while their wisdom teeth are removed. It is possible to perform surgery under local anesthesia only, or with intravenous sedation that helps the patient relax and blur the memories of the procedure. Although this is rather rare, it is possible to resort to general anesthesia, which requires hospitalization. The surgeon will explain the different options for anesthesia and will advise you, taking into account the importance of your surgery, your state of health and your level of apprehension regarding extraction. |
What are the potential complications ?As with any surgery, even well performed, there are risks associated with wisdom tooth extraction. Although complications are usually temporary, it is important to discuss them with your surgeon before extraction. |
InfectionAn infection can appear from a few days to a few weeks after surgery, and this in several ways:
Some signs are indicative of infection: pain, swelling, puffiness, bad taste in the mouth and fever. So if you notice the presence of these symptoms, consult your surgeon. He may prescribe antibiotics and possibly, under local anesthesia, remove the infected tissue. Older people and smokers are the most likely to suffer from an infection. |
Nerve injuryLower alveolar nerve A preoperative X-ray is very useful because it helps to assess the proximity of the low wisdom tooth to the nerve running in the bone under the roots of the teeth. The greater the proximity, the higher the risk of injuring the nerve by extracting the tooth. Impairment of the lower alveolar nerve is manifested by loss of sensitivity or numbness of half of the lower lip on the side of the affected nerve. Lingual nerve This nerve, running to the inner face of the lower jaw, passes close to the wisdom tooth and can also be damaged during an extraction. Lingual nerve involvement causes loss of sensitivity or numbness of the tongue on the same side as the affected nerve. You should know that most of the time, it is a temporary complication that resolves in a few weeks. In rare cases, the loss of sensation is final. |
Sinus ComplicationThe extraction of wisdom teeth in the upper jaw can have several consequences on the sinuses. Sinus communication: The extraction of the tooth can create a communication between the sinus and the oral cavity. The closer the tooth is to the sinus, the more likely it is to happen. The communication usually closes in a few weeks. However, it may happen that the communication does not close, which will require surgery. |
Dental damageDuring difficult extraction, adjacent teeth, particularly the 2nd molar, which is adjacent to the wisdom tooth, may be damaged. There may be a fracture, breakage of the restoration (filling), loosening of a crown or necrosis of the tooth, which will require root canal treatment. |
Broken toothSometimes the root of the 3rd molar that we are trying to extract is fragile and breaks. This is more common when the tooth has multiple roots and if they are curved. The surgeon may choose to retrieve this root tip or leave it in place, especially if the root fragment is near the inferior alveolar nerve. A residual root fragment usually causes no complications. |
Bone damageEspecially with deeply embedded teeth, the bone may be damaged. The bone around the 3rd molar can be damaged during extraction procedures. This is not alarming and there is no treatment to do. The bone will heal at the same time as the alveolus. |
Temporomandibular painThe temporomandibular joint may have been stressed during extraction and may be painful for a few days during movement.
In short, various complications are possible, but they are still rare. However, you must be informed to understand what surgery entails. |